WHITE PAPER
NeoNatalie Live - Impactful training on newborn resuscitation skills (2022)
Point of Contact: Laerdal Global Health Team - [email protected]
Introduction
Every year, nearly 900 000 babies around the globe die because they are not breathing at birth. Tragically, an even higher number are misclassified as stillborn, although they do have a heart activity during labor and could have been resuscitated.
The Helping Babies Breathe program was rolled out nearly 12 years ago. The program showed a significant impact when implemented in low-resource settings. However, research confirmed the opportunity to make further progress on survival rates for babies born asphyxiated, and in need of ventilation.
Through our partnership with Haydom Lutheran Hospital in Tanzania, we further addressed this challenge. As part of the Safer Births research project, we conducted a study recording data and videos from hundreds of resuscitations. This research included interviews with midwives and obstetricians from around the world.
Outcome
We learned 4 important things:
- Ventilation of the newborn was initiated too late. Even though the Golden Minute is common knowledge for health workers, almost no babies were ventilated within that first minute after birth.
- Ventilations were not given continuously. They were often interrupted with a lot of suction and stimulation.
- The newborn’s heart rate was not actively used to measure the effectiveness of the resuscitation. There is an important relationship between lung ventilation and heart rate which has been underemphasized.
- Newborns tend to be more difficult to ventilate than any training manikin currently on the market. Other newborn training manikins easily show chest rise when ventilation attempts are made which is not consistent with reality. During an actual medical event, there is often initial difficulties in ventilating asphyxiated newborns as their lungs are stiff and fluid-filled.
Solution
To address the challenges, we identified through our research, we embarked on creating a new, innovative tool. As such, we focused on some key elements for the development of a better and more realistic newborn training system:
- A training manikin that simulates the most common patient cases with respect to the full spectrum of ventilation difficulty. A manikin that more closely replicates real, asphyxiated babies, offering more resistance before the chest rise is visible.
- Software to measure and record the urgency (with regards to how quickly or slowly) the medical personnel are responding and conducting ventilations (during the training) with feedback on how the overall process went (post-training)
- Interconnectivity between the manikin and software to reinforce the importance of heart rate and lung ventilation
- A training system that meets two needs:
- Reinforcing practice of effective performance through auto-generated advice that was based on international guidelines.
- Is easy-to-use, readily available, and self-driven (not requiring an instructor). The training itself is short and repeatable as time for training and availability of instructors is limited, respectively.
Ultimately, the goal was to build confident and competent health workers who focused on delivering uninterrupted, continuous, and high-quality ventilation on non-breathing newborns.
This led to the development and delivery of NeoNatalie Live.
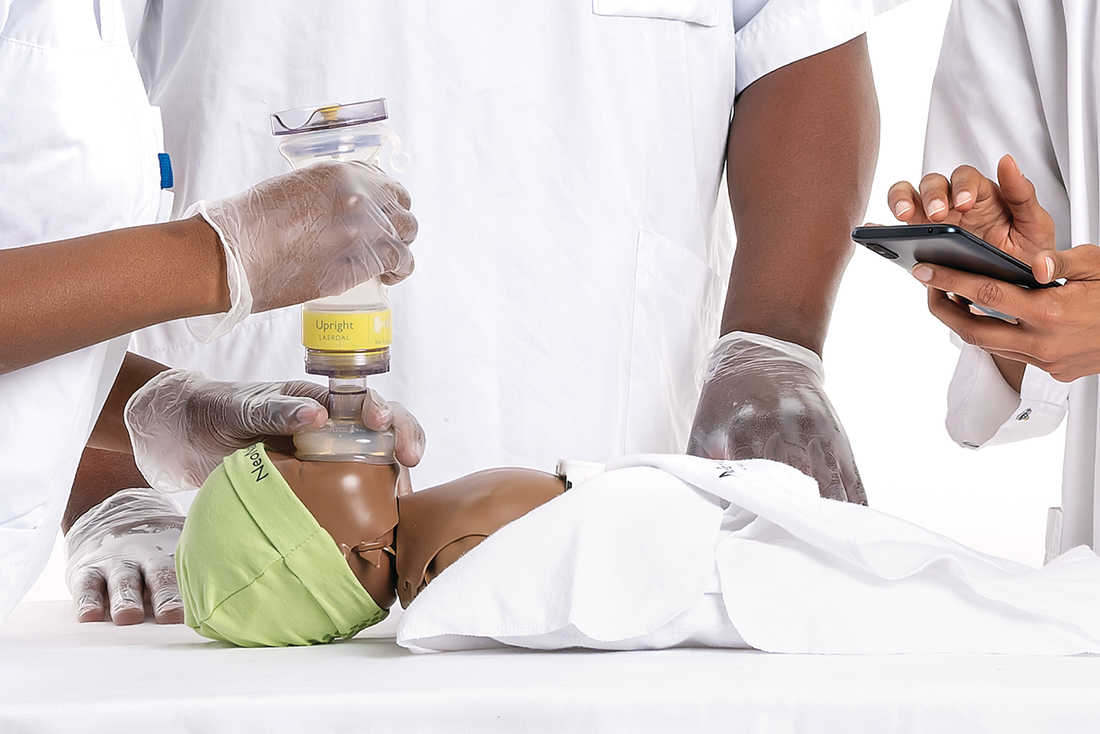
How was NeoNatalie Live made?
In continuation of the “Introduction” section, the development for NeoNatalie Live began in 2015 with a visit by the medical personnel from Tanzania to Laerdal offices in Norway. That meeting, as part of the Safer Births initiative, yielded more detailed focus on the “Outcomes” previously mentioned.
In due course, the conclusion was to make a newborn training manikin, like the original NeoNatalie, but with added functionality. A key difference being that this new solution provides both objective feedback on the resuscitation performance and it is more realistic for practicing actual, ventilation scenarios.
In further cooperation, improved training equipment for newborn resuscitation was continually refined and tested. The implementation expanded to include test locations in Nepal as well as Europe and the USA.
The finalized scenarios in NeoNatalie Live were based on more than 1200 resuscitation cases. Using this data ensures a closer modeling of realistic physiology in the manikin with respect to the actual, medical events. The totality of these features is included in the four, different patient cases in NeoNatalie Live.
Consequentially, NeoNatalie Live responds realistically to effective ventilation efforts including a chest rise increase, after initial resistance, and improving heart rate. Furthermore, it also includes a realistic, crying baby sound to signal spontaneous breathing after a successful resuscitation
The response of the manikin to learner performance is a key attribute. The following training behaviors are automatically measured by the manikin:
- Head positioning during ventilations with respect to correctly opening the airway
- Usage of a hand grip to ensure a good mask seal
- Ventilation rate
- Ventilation pressure
- Continuity of ventilations
To ensure both a self-driven learning experience as well as specific insights for improvement, it was determined to make sure this feedback was automated to the learner. For learners to improve, it was crucial to both know how they are doing and how to improve the ventilation technique.
With these challenges in consideration, our team developed an app that incorporates the elements measured in the manikin. Since availability of time and personnel often is constrained, the objective feedback is condensed into easily understandable advice for the learner. This encourages them on the pathway toward competent and confidence without being dependent on an instructor to assess the learner’s performance.
Furthermore, NeoNatalie Live encourages “Low-Dose, High-Frequency” training. Through training at more regular intervals in shorter sessions, health workers scale up their skills while avoiding degradation.

Implementation of NeoNatalie Live
The first prototype of NeoNatalie Live was finished in 2016.
Upon completion, it was introduced for testing at Haydom Lutheran Hospital in Tanzania. By 2017, additional prototypes were first installed at a hospital in Nepal before expanding to eight, more hospitals throughout the country. Though initially designed to be used in a low-resource setting, it has also had impactful installations for research purposes in the USA, Slovakia, and Norway, respectively.
With these additional sites, invaluable information was collected on both how the manikin was utilized by learners and elements of what could be improved. This includes extensive testing on the app to ensure both a user-friendly experience as well as a dynamic learner experience.
In 2021, the first NeoNatalie Live manikin was produced in Laerdal’s factory. The first set of manikins was sent to Tanzania for use in the Safer Births Bundle of Care Scale-Up. This batch went to 30 hospitals together with an early version of the NNL app. Promising preliminary results from Safer Births Bundle of Care recently led to the Global Financing Facility (GFF), a division of the World Bank, rewarding the project with additional funding for an even further scale-up. From 2023 the Safer Births Bundle of Care, including NeoNatalie Live, will scale-up to over 140 hospitals in five regions in Tanzania.[1]
Currently, with the help of our partners, more than 100 000 training sessions have been performed. Through the continuation of the existing projects, along with more user adoption now that it has been launched globally for purchase, the number of training sessions will rise.
In the next section, you will find a short summary and link to the full paper of research projects associated with NeoNatalie Live.
Supporting Research:
Novel Neonatal Simulator Provides High-Fidelity Ventilation Training Comparable to Real-Life Newborn Ventilation
Abstract:
Face mask ventilation of apneic neonates is an essential skill. However, many non-pediatric healthcare personnel (HCP) in high-resource childbirth facilities receive little hands-on real-life practice. Simulation training aims to bridge this gap by enabling skill acquisition and maintenance. Success may rely on how closely a simulator mimics the clinical conditions faced by HCPs during neonatal resuscitation. Using a novel, low-cost, high-fidelity simulator designed to train newborn ventilation skills, we compared objective measures of ventilation derived from the new manikin and from real newborns, both ventilated by the same group of experienced pediatricians. Simulated and clinical ventilation sequences were paired according to similar duration of ventilation required to achieve success. We found consistencies between manikin and neonatal positive pressure ventilation (PPV) in generated peak inflating pressure (PIP), mask leak and comparable expired tidal volume (eVT), but positive end-expiratory pressure (PEEP) was lower in manikin ventilation. Correlations between PIP, eVT and leak followed a consistent pattern for manikin and neonatal PPV, with a negative relationship between eVT and leak being the only significant correlation. Airway obstruction occurred with the same frequency in the manikin and newborns. These findings support the fidelity of the manikin in simulating clinical conditions encountered during real newborn ventilation. Two limitations of the simulator provide focus for further improvements.
Neonatal Resuscitation Skill-Training Using a New Neonatal Simulator, Facilitated by Local Motivators: Two-Year Prospective Observational Study of 9000 Trainings
Abstract:
Globally, intrapartum-related complications account for approximately 2 million perinatal deaths annually. Adequate skills in neonatal resuscitation are required to reduce perinatal mortality. NeoNatalie Live is a newborn simulator providing immediate feedback, originally designed to accomplish Helping Babies Breathe training in low-resource settings. The objectives of this study were to describe changes in staff participation, skill-training frequency, and simulated ventilation quality before and after the introduction of “local motivators” in a rural Tanzanian hospital with 4000–5000 deliveries annually. Midwives (n = 15–27) were encouraged to perform in situ low-dose high-frequency simulation skill-training using NeoNatalie Live from September 2016 through to August 2018. Frequency and quality of trainings were automatically recorded in the simulator. The number of skill-trainings increased from 688 (12 months) to 8451 (11 months) after the introduction of local motivators in October 2017. Staff participation increased from 43% to 74% of the midwives. The quality of training performance, measured as “well done” feedback, increased from 75% to 91%. We conclude that training frequency, participation, and performance increased after introduction of dedicated motivators. In addition, the immediate constructive feedback features of the simulator may have influenced motivation and training quality performance.
A Randomised Controlled Study of Low-Dose High-Frequency In-Situ Simulation Training to Improve Newborn Resuscitation
Abstract:
Positive pressure ventilation of the non-breathing newborn is a critical and time-sensitive intervention, considered to be the cornerstone of resuscitation. Many healthcare providers working in delivery units in high-resource settings have little opportunity to practice this skill in real life, affecting their performance when called upon to resuscitate a newborn. Low-dose, high-frequency simulation training has shown promise in low-resource settings, improving ventilation performance, and changing practice in the clinical situation. We performed a randomized controlled study of low-dose, high-frequency simulation training for maintenance of ventilation competence in a multidisciplinary staff in a busy teaching hospital in Norway. We hypothesized that participants training according to a low-dose, high-frequency protocol would perform better than those training as they wished. Our results did not support this, although the majority of protocol participants were unable to achieve training targets. Subgroup analysis comparing no training to at least monthly training did identify a clear benefit to regular simulation practice. Simulated ventilation competence improved significantly for all participants over the course of the study. We conclude that frequent, short, simulation-based training can foster and maintain newborn ventilation skills in a multidisciplinary delivery unit staff in a high-resource setting
Use of a Novel Manikin for Neonatal Resuscitation Ventilation Training
Abstract:
All providers who attend deliveries independently should be well versed in the performance of effective ventilation, assessment of the quality of ventilation/interventions supplied and able to troubleshoot in situations where these may be ineffective. A novel manikin serves as a unique ventilation-focused training tool to practice these clinical skills and decision-making. The data generated by the manikin, with the aid of a facilitator, may be used for formative and summative feedback on an individual level or curricular development on a larger level. This communication describes the importance of focused ventilation training for front-line providers and illustrates how this manikin can be incorporated into an individualized ventilation training program.
Innovations in Cardiorespiratory Monitoring to Improve Resuscitation With Helping Babies Breathe
Abstract:
Ninety percent of intrapartum-related neonatal deaths are attributable to respiratory depression, with the vast majority of these deaths occurring in low- and lower middle–income countries. Neonatal resuscitation training with Helping Babies Breathe (HBB) decreases mortality from respiratory depression. Cardiorespiratory monitoring in conjunction with HBB can provide valuable resuscitation feedback for both training and bedside purposes. In this article, we discuss 3 innovations that couple cardiorespiratory monitoring with HBB: NeoNatalie Live, the Augmented Infant Resuscitator, and NeoBeat. NeoNatalie Live is a high-fidelity manikin that facilitates bag mask ventilation training through case scenarios of varying difficulty. The Augmented Infant Resuscitator is added in-line between a face mask and ventilation bag during bag mask ventilation training to provide users with real-time feedback on ventilation quality. NeoBeat is a battery-operated heart rate meter that digitally displays the newborn heart rate during bedside resuscitations. For each innovation, we review details of the device, implementation in the field, and areas for further research. Using early experience implementing these devices, we suggest building blocks for effective translation of training into improved care. We also highlight general challenges in implementation of devices in facilities in low- and lower middle–income countries including considerations for training, adaptations to existing workflow, and integration into the ecosystem. Although the devices highlighted in this article hold promise, more data are needed to understand their impact on newborn outcomes.
Effect of skill drills on neonatal ventilation performance in a simulated setting- observation study in Nepal
Abstract:
Maintaining neonatal resuscitation skills among health workers in low-resource settings will require continuous quality improvement efforts. We aimed to evaluate the effect of skill drills and feedback on neonatal resuscitation and the optimal number of skill drills required to maintain the ventilation skill in a simulated setting.